When to Stop Burping Infant: Simple Signs
We may earn a commission for purchases made using our links. Please see our disclosure to learn more.
You’re in that phase where feeding feels like a whole production: latch/bottle, pause, burp, spit-up cleanup, outfit change (for both of you), repeat. And at some point you start wondering, when to stop burping infant… because surely this “tiny-human wind management” job can’t be forever, right?
Good news: for most babies, it does get easier—often somewhere around 4–6 months, when their digestive system matures and they’re moving more, sitting with support, and swallowing less air.
But (because babies love being unique) the real answer isn’t only about age—it’s about signs.
In this guide, you’ll learn what to watch for, how to adjust burping as your baby grows, what’s normal vs. “call your pediatrician,” and a few practical tools that make the whole thing less messy.
Burping 101: Why Babies Need It in the First Place
Babies swallow air while feeding. Some do it a little. Some do it like they’re trying to win a competitive sport. That air can sit in the stomach and make them uncomfortable, fussy, or more likely to spit up.
Pediatric guidance often suggests burping during natural breaks (like switching breasts or pausing a bottle) and again at the end—especially early on.
The Big Question: When to Stop Burping Infant (The Short Answer)
Most babies outgrow the need for routine burping around 4–6 months, but some can ease off earlier, and some benefit from longer.
Here’s the vibe I want you to hold onto:
You’re not “quitting burping.” You’re “graduating to burping only when it helps.”
The Age-by-Age Guide (So You Have a Starting Point)
Newborn to 2 months: “Burp is still your co-pilot.”
Many newborns do best with frequent burp breaks, especially bottle-fed babies.
2 to 4 months: “Start experimenting.”
Some babies still need it every time. Others only need it when they’re gulping, squirmy, or pulling off.
4 to 6 months: “Most babies can taper.”
This is the most common window where you can reduce routine burping.
6 months and up: “Burp breaks become occasional.”
If your baby is sitting more, eating solids, and generally less gassy from feeds, you may only burp when they seem uncomfortable.

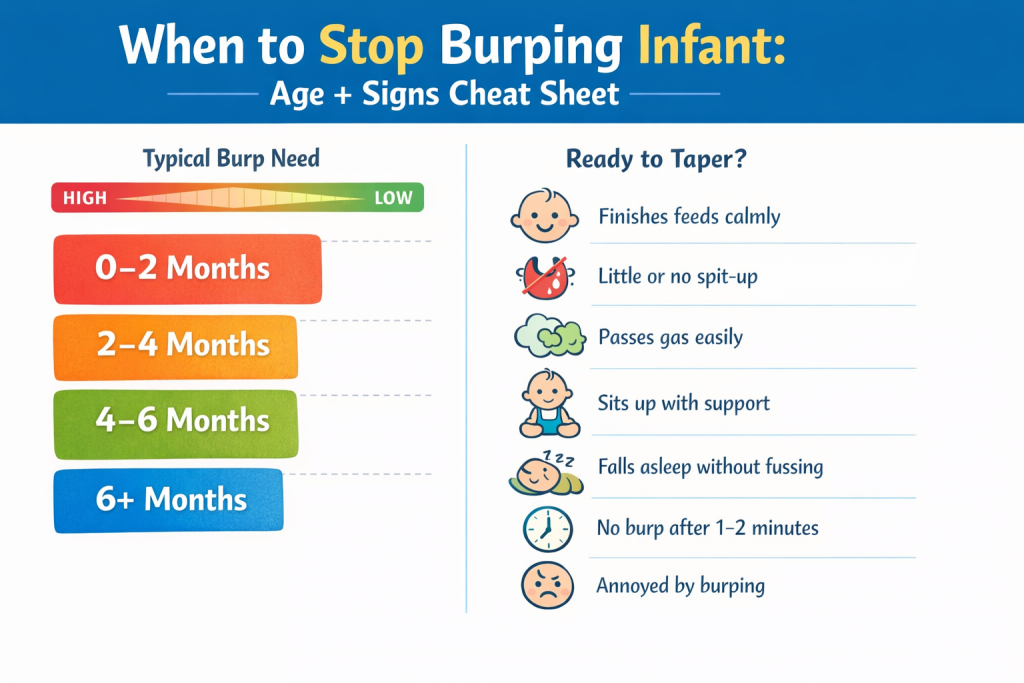
7 Simple Signs Your Baby Doesn’t Need Burping Every Time
If you’re seeing several of these consistently, you can start tapering:
- They finish feeds calmly and don’t squirm or pull away
- They don’t spit up much (or spit-up doesn’t bother them)
- They pass gas easily on their own (yes, that counts as a skill 😄)
- They can sit with support or move around more after feeds
- They fall asleep after feeding without waking from discomfort
- Burping attempts rarely produce a burp (even after a minute or two)
- They seem more annoyed by the burp interruption than helped by it
When to Keep Burping (Even If They’re “Older”)
Some babies benefit from longer-than-average burping if they:
- gulp quickly or get very eager at the bottle/breast
- have frequent spit-up or reflux symptoms
- get fussy right after feeding
- are switching formulas or bottle types
- tend to get gassy in the evenings (the classic “witching hour”)
Cleveland Clinic also notes that not every baby burps every time—and recommends keeping attempts short to avoid frustration.
Breastfed vs Bottle-Fed: Does It Change When You Stop?
Often, yes—a little.
Breastfed babies
Some swallow less air and may need fewer burps.
Bottle-fed babies
Bottle feeding can introduce more air depending on bottle shape, nipple flow, and pacing. Burping may stay useful longer for some bottle-fed babies.
No matter how you feed, your baby’s comfort matters more than a rigid schedule.
Night Feeds: Should You Still Burp at 2 A.M.?
This is where parents get spicy (understandably). Here’s a gentle middle path:
- If your baby is gulping, pulling off, or seems uncomfortable → do a quick burp.
- If they’re sleepy, calm, and feeding smoothly → you can try a short, low-effort burp (30–60 seconds), then back down.
And if you try and nothing happens? It’s okay to stop—Cleveland Clinic suggests just a minute or two max.
How Long Should You Try to Burp Before Calling It?
A helpful rule: 1–2 minutes.
After that, you’re often just doing interpretive dance with a baby on your shoulder.
If there’s no burp and your baby seems comfortable, you can move on.

Gentle Burping Techniques That Still Work as Baby Grows
Over-the-shoulder
Best for big burps, especially after bottles.
Sitting upright, leaning forward
Great once baby has more head/neck control.
Face-down on your lap
Works well for some babies who hate shoulder burping.
If your baby spits up while burping, that’s common—keep a cloth handy and try not to take it personally.
The “Spit-Up vs Vomit” Difference (So You Don’t Panic)
Spit-up is usually effortless and small. Vomiting is more forceful.
If you’re seeing poor weight gain, blood, green fluid, breathing trouble, or severe discomfort, that’s a call-your-pediatrician situation.
Also: reflux often peaks around 4–5 months and improves by 9–12 months in many babies.
Common Mistakes That Make Burping Harder
- Burping too aggressively (tiny backs don’t need drum solos)
- Waiting until baby is very upset before pausing
- Using a nipple flow that’s too fast (gulping = more air)
- Trying for too long and turning it into a battle
If feeding feels like a race, slow it down. Babies aren’t impressed by speed.
A Simple “Taper Plan” If You’re Ready to Stop Routine Burping
Try this for 3–5 days and see how your baby responds:
- Keep the mid-feed burp (or breast switch burp).
- Skip the end burp if baby finishes calm and drowsy.
- If fussiness/spit-up increases, bring back the end burp for a bit.
- If things stay smooth, taper further: burp only when baby shows discomfort.
This way, you’re not guessing—you’re running a tiny, parent-led experiment.
Red Flags: When Gas or Burping Issues Need a Check-In
Call your pediatrician if you notice:
- persistent, inconsolable crying with feeds
- feeding refusal
- poor weight gain
- blood in spit-up or stool
- frequent choking/coughing with feeds
- projectile vomiting
Trust your instincts. You’re with your baby the most—you’ll spot patterns before anyone else.
🔹 Product Section: Helpful Gear for Burp Season
1) Burt’s Bees Baby Organic Cotton Burp Cloths (5-Pack)
- Short description: Soft, absorbent, generous coverage—great for spit-up days.
- Features: Organic cotton, larger size, multi-pack convenience.
- Best for: Parents who want fewer outfit changes (for themselves).
2) Boppy Nursing Pillow (Feeding Support Pillow)
- Short description: Helps position baby comfortably so feeds are calmer (often less gulping, less air).
- Features: Ergonomic shape, washable cover, designed for multiple feeding holds.
- Best for: Breastfeeding, bottle-feeding, and your shoulders.
3) Philips Avent Anti-Colic Baby Bottles
- Short description: Designed to reduce air ingestion—handy if burping feels endless.
- Features: Anti-colic valve, wide neck, easy cleaning.
- Best for: Babies who get gassy with standard bottles.
4) Mylicon Infants Gas Relief Drops (Simethicone)
- Short description: A common option parents ask about for gas discomfort.
- Features: Dye-free option, dosing syringe, can be used as directed.
- Best for: “Baby looks uncomfortable but won’t burp” moments.
5) Frida Baby Windi Gas Passer
- Short description: For occasional, “we’ve tried everything” trapped-gas scenarios.
- Features: Designed for quick gas release; follow instructions carefully.
- Best for: Rare use—when baby is clearly uncomfortable and nothing else works.
And for the constant laundry rotation phase (spit-up + drool + milk drips = daily costume changes), here’s a cozy, practical read on organic baby clothes that stay gentle on sensitive skin.
🧪 What Research and Experts Say About Burping (And When to Stop)
Here’s the reassuring part: some trusted sources explicitly say there aren’t hard rules—and that you should follow your baby’s cues.
Study #1: Burping may not prevent colic (and may increase spit-up)
A randomized controlled trial found burping didn’t significantly reduce colic, and it was associated with more regurgitation episodes in healthy infants followed up to 3 months.
What this means for you:
If you’re doing everything “right” and burping still feels pointless, you’re not failing. Some babies simply don’t benefit much from routine burping—and that’s exactly why watching your baby’s signs matters.
Expert guidance: Follow cues, keep it simple, don’t force it
The NHS points out there are no strict rules for when to burp—some babies need it during feeds, others after, and cues matter.
And HealthyChildren.org (AAP) shares practical burping basics and suggests frequent burping as something you can try—especially early on.
Bottom line: As your baby grows, it’s reasonable to taper—and if burping isn’t helping, you can stop making it a mandatory step.
FAQ
When to stop burping infant at night?
If your baby feeds calmly and stays sleepy, try a brief 30–60 second burp or skip it. If they squirm, pull off, or seem uncomfortable, do a quick burp.
When to stop burping infant after breastfeeding?
Many breastfed babies need fewer burps. You can start tapering when your baby finishes relaxed, doesn’t seem gassy, and burps rarely happen even when you try.
When to stop burping infant after bottle feeding?
Bottle-fed babies may swallow more air depending on nipple flow and pacing. You can taper when feeds are smooth, baby isn’t fussy after, and spit-up doesn’t increase when you skip routine burps.
Is it okay if my baby doesn’t burp every time?
Yes. Some babies don’t burp at every feed. If your baby seems comfortable and settles well, it’s fine to move on after a short attempt.
When should I worry about gas or reflux instead of burping?
If your baby has poor weight gain, feeding refusal, blood in spit-up/stool, breathing issues, or projectile vomiting, call your pediatrician. Reflux often peaks around 4–5 months and improves over time, but red flags deserve a check-in.
Conclusion
If you’ve been waiting for a clear “you may stop burping now” announcement—consider this your permission slip (with a tiny asterisk).
Most babies can taper burping around 4–6 months, but the best answer is the one your baby shows you: calmer feeds, fewer gas cues, and less benefit from the burp break.
So try the taper plan. Watch how your baby responds. Keep what helps, drop what doesn’t.
And remember: you’re not “behind” if your baby still needs burping sometimes. You’re just parenting a real human—one burp, giggle, and spit-up surprise at a time.




